- Call 07 3805 3223
- Find us on Facebook
- Follow Us
- Book Appointment
Endometriosis is a condition whereby cells that are usually found inside the uterus decide that they want to grow outside of the uterus. Generally on the outside wall, ovaries, fallopian tubes, and other organs in the pelvis but the lesions can be found on the diaphragm or even the brain!! These cells continue to act like they are in the uterus under the effect of the hormone estrogen in a women’s monthly cycle – they breakdown and bleed, and then scar.
Pelvic pain can vary through the monthly cycle but does not necessarily directly relate to the stage of the condition.
Initially, a hour long consultation with our women’s health physio can help you with your pelvic pain. An internal examination may be required to assess your pelvic floor and it’s function. A further plan will be determined at the first session and will vary between twice weekly sessions, to once a week or fortnight, depending on your symptoms and requirements.
As exercise is a proven method of assisting with pelvic pain from endometriosis (reducing the amount of estrogen and therefore reducing pain symptoms), appointments with an exercise physiologist will get you on the right track to manage your symptoms. Helping to train the pelvic floor, lengthening tight abdominal muscles are some of the specific ways exercise can help. Additionally global muscle strengthening and cardiovascular exercises will improve symptoms and quality of life.
Coming soon…
Coming soon…
Coming soon…

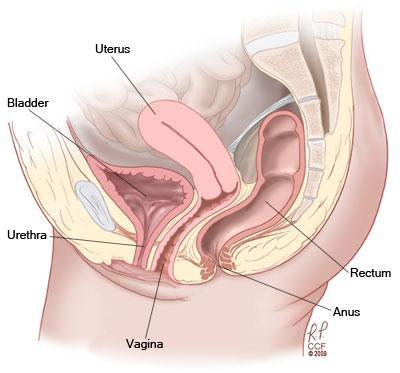
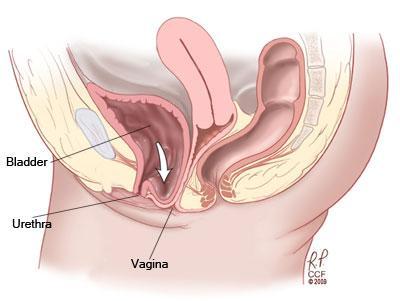
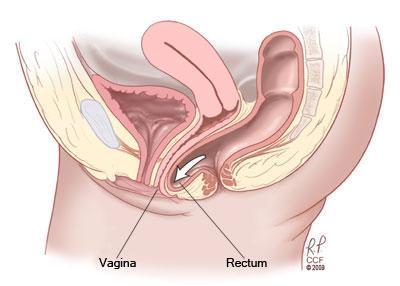
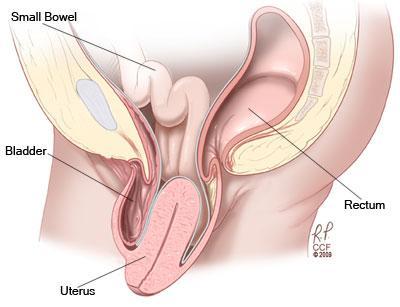
Pelvic organ prolapse is the condition where one or more of the organs in the pelvic cavity – the bladder, uterus or rectum – descend, resulting in a protrusion into the vagina. There are 3 types of prolapse, and women may experience one, two or three of these at the same time:
Symptoms of prolapse include:
Typically treatment starts with an initial assessment that takes 1 hour (either a 1 hour block or 2 x ½ hour appointments held on consecutive, or near consecutive, days). The assessment will involve your physiotherapist asking lots of questions regarding your symptoms, bladder, bowel & sexual function, followed by an internal vaginal examination to assess the function of your pelvic floor and the extent of the prolapse. From there your therapist will discuss your further treatment – which may involve pelvic floor exercises, lifestyle recommendations, pessary fitting or a combination of these. Usually you will have a follow up appointment in 1-4 weeks, with 2-3 further follow up appointments. The interval between these can vary from 1-2 weeks to 3 months depending on the progress that is being made.
If a pessary is to be fitted, and hour long appointment is required to determine the size needed and to ensure you are able to manage the pessary yourself. It is a requirement of our profession that there is a follow-up appointment 1-2 weeks after fitting, with ongoing reviews every 3 months.
Our women’s health physiotherapist, Julie.
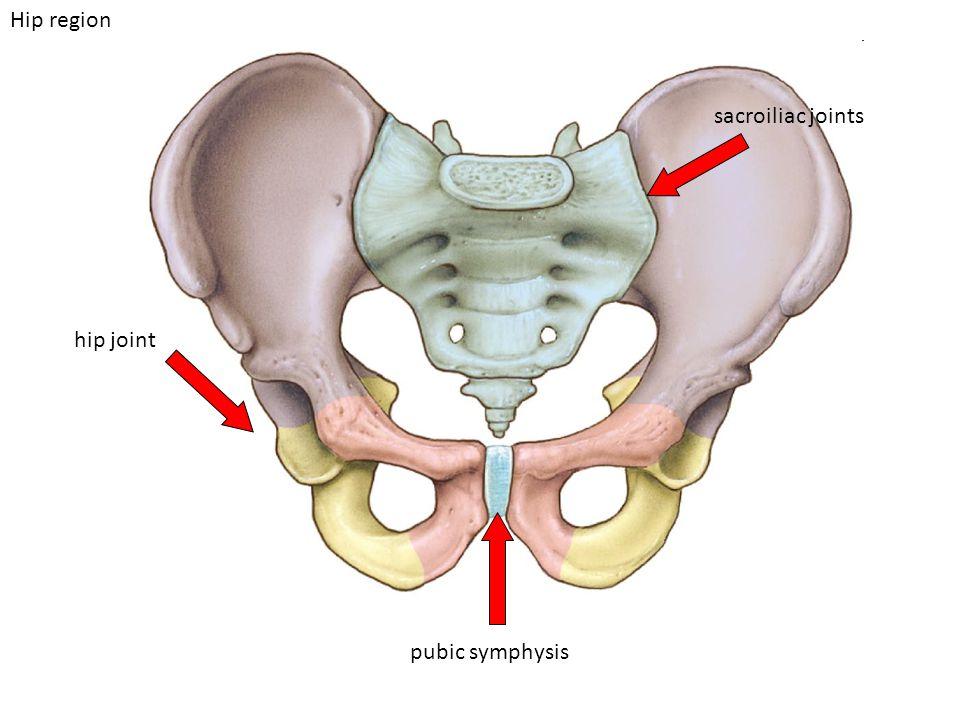
Pelvic Girdle Pain is pain experienced in the joints of the pelvis – around the back where the pelvis joins the tailbone (the sacroiliac joints, or SIJs) and/or around the front where the two sides of the pelvis join (the pubic symphysis). It is likely to cause pain during things like walking, using stairs, rolling in bed, standing on one leg, standing with legs wide or getting in & out of cars. It usually starts in the latter stages of the 2nd trimester or into the third trimester.
It is important to note that Pelvic Girdle Pain is not the same as Pelvic Pain – which is related to the soft tissues and organs inside the pelvis and is related to pelvic floor muscle dysfunction.
During pregnancy, the body releases hormones that help relax the ligaments that support the joints of the pelvis, which is what allows the pelvis to expand enough to deliver the baby when the time comes. Sometimes this causes excessive movement at these joints which then rub & become irritated. Changing muscle function and posture as pregnancy progresses also contributes, as does any pre-existing weakness, not to mention the increased load as the baby grows.
We can release tight muscles that may be spasming and causing further dysfunction at the joint. We also teach exercises to help support the joints better and movement strategies to help avoid placing excessive stress on the joints. In some cases we may also prescribe a specific belt that helps support the joints.
Typically we see patients once a week for 3-4 weeks to alleviate pain, release muscles and teach exercise progressions. Some ladies elect to continue with weekly or fortnightly maintenance visits as their pregnancy progresses, it really comes down to how each individual is responding and how the pregnancy is going. You will have the opportunity to discuss treatment plan options with your therapist to determine what will be the best solution for you.
Our women’s health physiotherapist, Julie
Coming soon…

Urinary urgency is that sudden, unexpected, strong need to empty your bladder that comes on out of the blue, and you feel like you must get to the bathroom immediately. When that urge results in leaking it is called Urge Incontinence.
Urgency can be a condition unto itself, or it can be a symptom of other conditions (such as Bladder Pain Syndrome or Urinary Tract Infections to name a couple).
Urgency often comes together with increased frequency – where you are emptying your bladder too many times a day.
Urgency can occur for a number of reasons. It can be the result of bladder spasms, dysfunction in parts of the nervous system that give the signal to empty your bladder, or in many cases, its developed as a result of some of our own behaviours & habits.
We can help with learning strategies to calm down the urge, adjusting behaviours, and improving pelvic floor function.
Your initial visit will be an hour long, as there are a lot of details about bladder, bowel and pelvic function that we need to go through in order to work out the nature of your problem. It is likely your therapist will recommend an internal vaginal examination to check your pelvic floor function. You will also be asked to complete a 48 hour bladder diary so we can get a picture of what your bladder is up to.
Follow-up visits can be 20-30 minutes depending on what we find, and at your second visit we will be able to go through the findings of the bladder diary, and make recommendations about how to address what is found. Usually we follow up 3-4 weeks after this with a repeat bladder diary to see how the treatment is progressing.
Our women’s health physiotherapist, Julie.